The Financial Impact of Patient Engagement Technology
April Fool’s Day in 2016 came as no joke for the nearly 800 hospitals that became impacted by the Comprehensive Care for Joint Replacement (CJR) ruling, a new bundled payment model for lower extremity joint replacement. It doesn’t take reading the more than 600 page ruling to uncover that one of the underlying themes is to engage the patient throughout the entire episode of care by encouraging better coordination among hospitals, physicians, and other providers. Whether or not a hospital is participating in CJR now or in the future, patient engagement throughout an episode of care must become a priority. Not only is it the right thing to do for patients, it now also has a significant impact on the bottom-line.
Under CJR, Medicare will begin paying hospitals based on a “target price” for all related joint replacement services within a 90-day episode of care. Medicare will reconcile the actual spending against the target price. To determine whether or not a hospital is eligible to receive reconciliation payments and receive maximum reimbursement, Medicare will evaluate performance on three quality measures: complications, patient experience, and patient reported outcomes.
The financial impact as a result of performance on these quality measures is significant. If the composite score of the three quality measures is “below acceptable,” the hospital will not receive reconciliation payments, even if cost measures fall below the target price. Based on ranking, the composite scores also determine the percentage that a hospital will be reimbursed or has to pay. Whether impacted by CJR or not, performance on these and other quality measures matter, especially for the bottom-line.
A VOX study further demonstrates how critical successful quality measures are. VOX’s OrthoCare web-based program was used to engage the patient 30 days pre-op through 90 days post discharge and provided the patient with educational content including text, video, interactive preparation tools, and patient reminders. The study concluded economic improvement of such engagement can exceed $1,000 per patient.
Few would argue against the claim that patients who are engaged as decision-makers in their care tend to be healthier and have better outcomes. Not all outcomes can be directly tied to a dollar amount, but the VOX Telehealth study found that use of the OrthoCare program led to improvement among several of the indicators that can lead to improved cost of care, including increased direct- to-home discharges, reduced length of stay, and fewer readmissions.
In fact, results from the study showed more than a 10 percent increase in direct-to-home discharges versus a post acute destination, approximately a half-day average length of stay improvement, and more than a 1 percent reduction in readmission rates.
Applying these improvements to a sample health system that conducts 500 procedures per year, the table below illustrates how improvements in these measures can impact a hospital’s bottom line by greater than $500,000 annually or more than $1,000 per patient.
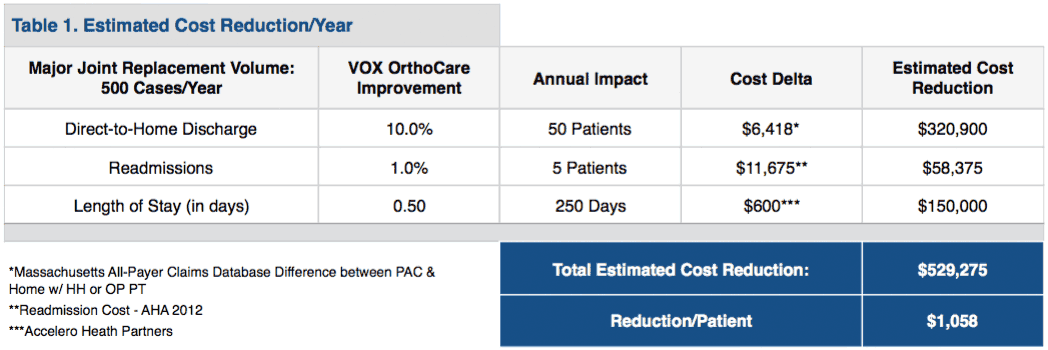
These results should come as no surprise. Optimal surgery preparation, less time spent in the hospital, and being discharged home directly after surgery will result in a positive outcome. Additionally, the ability to ask patients questions critical to proper recovery and being able to proactively direct them to the right resources if trouble arises after surgery will prevent avoidable readmissions.
While not actively tracked during the study, it is anticipated that patient engagement software like VOX’s could also have a direct or indirect impact on several other markers that either improve net revenue or decrease cost of care. These include:
- Reduced length of stay at skilled nursing or other post acute facilities
- Decreased home health utilization via patient participation with online rehabilitation programs and interactive risk assessments
- Fewer surgical cancellations through improved patient preparation
- Expanded case capacity by improving clinical workflow and hospital bed availability
- Improved market share through program differentiation
- Increased referrals from primary care physicians by creating a better experience for their patients
- Value based purchasing incentives for tracking and achieving outcomes based quality care measures
- Improved staffing utilization via better patient management
Although patient engagement strategies aimed at improving these various targets seem like common sense, few hospitals have the staffing to continuously engage their patients in such a manner.
Using OrthoCare’s innovative technology, hospitals can optimize patient participation by virtually holding a patient’s hand throughout the episode of care to remove gaps in the care continuum. For patients, who often have to go weeks between visits with the hospital or their doctors prior to or after surgery, VOX connects all touch points that occur throughout the episode of care, making them feel less isolated from their providers.
When implemented, patient engagement technology, such as VOX’s, has the ability to improve care coordination, improve patient outcomes, and aid providers in delivering a better patient experience. With changing reimbursement models and greater focus on quality measures, its financial impact is undeniable.
For more information about VOX Telehealth and its orthopedic platform, the OrthoCare Program, please contact [email protected].
About the Author
Philip Feldstein is Vice President of Ortho Solutions at VOX Telehealth and brings more than 10 years of experience in orthopedic service line management. Throughout his career, Phil has worked with more than 100 hospitals, physician groups, and other outpatient ancillary service providers to develop strategies for optimizing care, while balancing the financial and volume growth. Phil has held senior roles in marketing strategy and business development in numerous leading orthopedic organizations. Phil earned a BA from Indiana University and an MBA from the University of Illinois in Chicago.
About VOX Telehealth
VOX Telehealth was founded to improve patient outcomes by redefining the patient experience and recovery model. Through a state-of-the art platform, VOX delivers procedure-specific, full episode-of-care engagement solutions that provide education, coordination, and monitoring through industry leading content, proprietary SmartTasks™ and a customizable alert escalation and notification system. Engaging the patient throughout their pre-op phase, as well as through transition of care and recovery, patients are connected and accountable, leading to greater satisfaction, improved outcomes, and reduced cost of care. For more information, visit www.voxtelehealth.com.